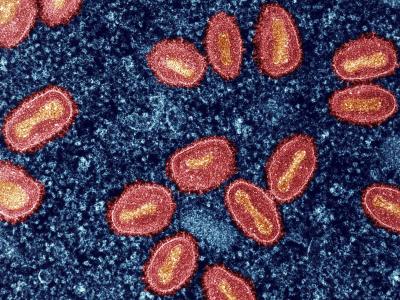
Study finds antibiotic resistance in US, UK Campylobacter holding steady
A large-scale analysis reveals that the prevalence of antimicrobial resistance (AMR) has remained stable for Campylobacter in the United States and United Kingdom in recent years, suggesting that antibiotic stewardship efforts have not made a large impact, according to a new study in Antimicrobial Agents and Chemotherapy.
UK and US scientists analyzed 32,256 Campylobacter jejuni and 8,776 Campylobacter coli genomes taken from people, poultry, and other farm animals, comparing trends in 2015 through 2018 with those in 2001 through 2014, a period that served as a baseline. UK samples were dominated by human isolates (about 70% for C coli, for example, versus 5% for US C coli), with farm animal samples poorly represented. In contrast, US samples showed a better representation of farm animal samples for both C jejuni and C coli.
The team founds that AMR markers were detected in 68% of C coli and 53% of C jejuni isolates, with 15% of C coli isolates being multidrug resistant, compared with only 2% of C jejuni isolates. The prevalence of aminoglycoside, macrolide, quinolone, and tetracycline resistance remained fairly stable from 2001 to 2018 in both pathogens, but statistically significant differences were observed between the two countries. For example, the proportion of aminoglycoside- and tetracycline-resistant isolates was significantly higher in the United States than in Britain from 2015 to 2018, while the prevalence of quinolone resistance was significantly lower in the United States.
The authors conclude, "Taken together, the data presented here strongly suggest that reduced usage of antibiotics has not resulted in a significant reduction of antimicrobial resistance in Campylobacter, which is of considerable public health and economic concern.
"Changes in agricultural practices, slaughter, and retail will need to be substantial to reduce the overall prevalence of Campylobacter. These efforts should lessen the need for antibiotic usage to achieve the goals of antimicrobial stewardship."
Apr 11 Antimicrob Agents Chemother study
Study highlights risk of discharged C diff patients spreading the disease
The incidence of Clostridioides difficile infection (CDI) in household members exposed to a recently CDI-hospitalized family member was 73% greater than for those not exposed, and the incidence increased the longer the family member was in the hospital, University of Iowa researchers note today in a study in Emerging Infectious Diseases.
CDI is one of the most commonly occurring types of healthcare-associated infections and is predominantly associated with hospital stays. Occurring mainly in people who've had both recent medical care and antibiotic exposure, it is considered an urgent antibiotic resistance threat by the Centers for Disease Control and Prevention and affects 223,000 US hospital patients a year.
The investigators analyzed US insurance claim data from 2001 through 2017 to compare monthly CDI incidence among people in households with and without a family member hospitalized in the previous 60 days. They found that CDI incidence among insurance enrollees exposed to a recently hospitalized family member was 73% greater than enrollees not exposed
The researchers also identified a relationship between the total days of hospital stay for the index patient and the CDI risk in family members. Compared with people whose family members were hospitalized less than a day, the incidence rate of CDI in household contacts increased from 1.30 (95% confidence interval [CI], 1.19 to 1.41) for 1 to 3 days of hospitalization to 2.45 (95% CI, 1.66 to 3.60) for more than 30 days of hospitalization.
The authors conclude, "Asymptomatic C. difficile carriers discharged from hospitals could be a major source of community-associated CDI cases."
Apr 13 Emerg Infect Dis abstract